Does your zip code define your life expectancy?
Given his history, Denny Witkowski, 80, is in a good place today. Diagnosed with congestive heart failure years ago, he has been hospitalized several times — but since his last stay, in November, he has been home with his wife, Thelma.
His condition is stable, and he’s enjoying life.
“I’m more comfortable being here,” Witkowski said when The Journal visited him recently. “My health is much improved.”
For that, he can credit Integra Community Care Network, a service of Care New England, South County Health and other groups. Working with a patient’s doctors, specialists, labs and other health-care entities, Integra professionals can provide hospital-level care in a person’s home — at reduced cost and with the comfort Witkowski appreciates.
Nurse care manager Jean E. White coordinates Witkowski’s care. She worked at Care New England's Kent Hospital for 25 years before joining Integra four years ago.
“This allows us more time to make sure folks have what they need,” she said. She or another team member is available around the clock, a telephone call away.
“It feels so good, 24/7,” Thelma said.
“They know what’s going on,” said Witkowski, owner for many years of Warwick Dental Laboratory. "That's the big thing. It’s the best thing that ever happened to me.”
Were he living in another state, Witkowski might not faring as well.
That conclusion may be drawn from the authoritative 2019 “Scorecard on State Health System Performance,” a measure of access to and quality of health care, outcomes and disparities in each of the 50 states and the District of Columbia.
Rhode Island ranks seventh in the nation according to the scorecard, published annually by the nonpartisan Commonwealth Fund and based on analysis of data from several nonprofit and government sources. Only Hawaii, best in the nation, and Massachusetts, Minnesota, Washington state, Connecticut and Vermont ranked higher. (Texas, Oklahoma and Mississippi, worst in America, held the bottom three places.)
But good results don’t come cheap.
In its latest analysis of health-care expenditures for most services and products such as pharmaceuticals, the Kaiser Family Foundation in 2014 determined that Rhode Islanders spent $9,551 per person annually, 10th-highest in the United States. A more recent Kaiser report, in 2017, found $8,352 in spending per person from state and federal sources such as Medicaid and Medicare.
While Rhode Island's overall scores were well above the national average for health-care delivery and health outcomes, The Commonwealth Fund this year found deficiencies.
“Potentially avoidable emergency department visits” for people 65 and older — a costly hospital visit for treatment that likely could have been provided by a visit to a doctor or urgent-care center — rose, dropping Rhode Island to 40th place nationally. Adult obesity worsened, leaving Rhode Island with a rate above the national average.
And drug-poisoning deaths — essentially, by overdose — increased, to a rate of 21.7 deaths per 100,000 residents, the ninth-highest rate in the country. (That statistic is derived from three-year-old data; drug overdose deaths in the state declined in 2017 and 2018. Nonetheless, the Health Department declares, “drug overdose deaths in Rhode Island are a public health crisis.” Last year, 314 drug overdose deaths occurred in the state.)
Speaking recently with The Journal, state Department of Health deputy director Ana Novais referenced two graphs she often cites to illustrate Rhode Island’s state of health.
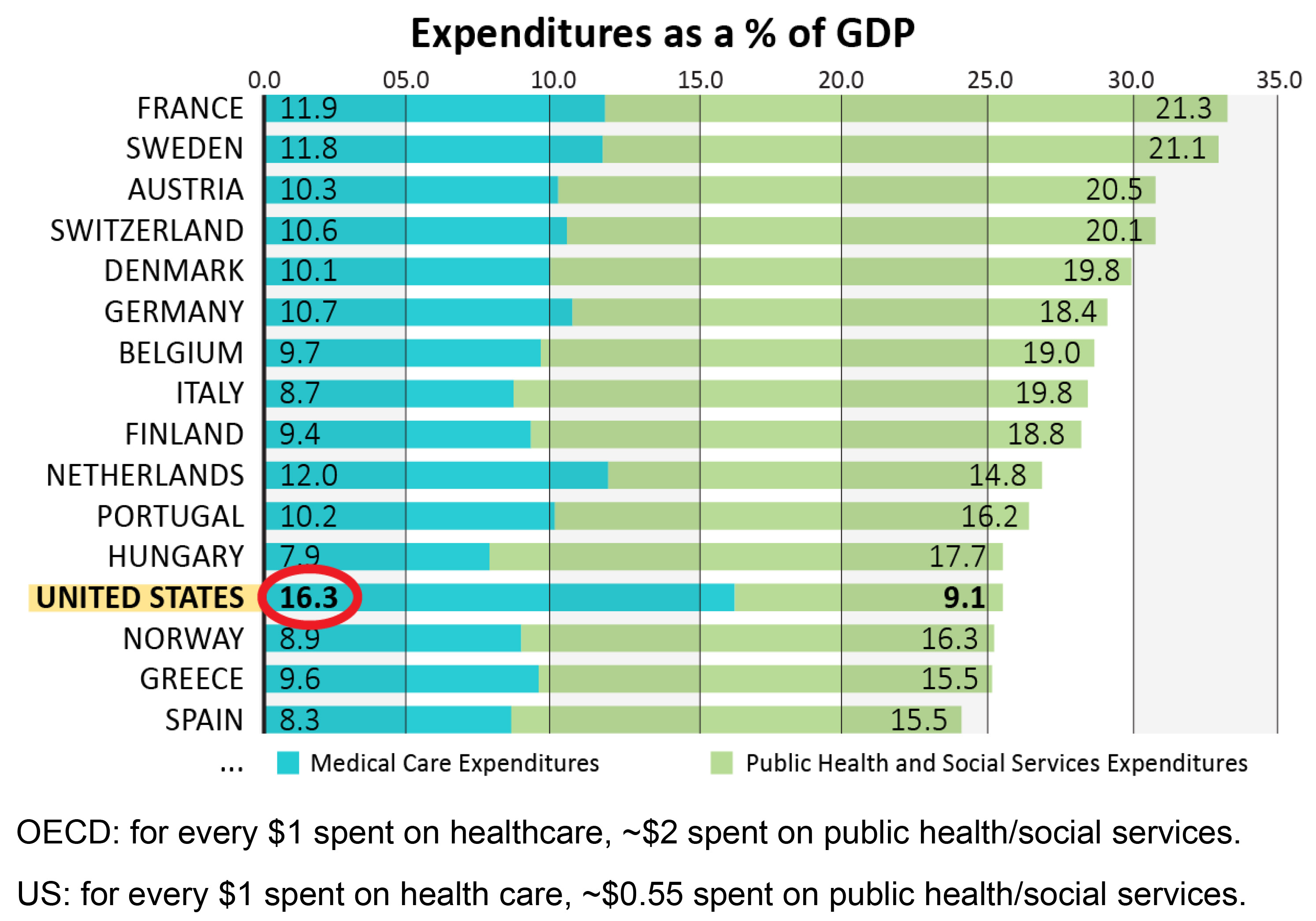
The first compares many countries’ health-care spending with life expectancy: the United States spends the most by far of any nation, yet has a lower life expectancy than many other countries. The second charts spending in health services against social services: while the United States is tops in health-care spending, it ranks low in social-service investments.
The correlation is apparent — and it applies not only to the United States generally, but also to individual states, including Rhode Island, according to Novais.
“It’s the issue of how we spend money,” she said.
Pharmaceuticals, technology, hospitalization, bureaucracy — these are among the drivers of direct health-care spending, where America leads the world. Despite spending less, countries including France, Germany and Italy achieve superior outcomes — and that can be attributed to more investment in social services including education, housing and non-medical government assistance, Novais said.
“The reality is if you look at the life outcomes of one individual, health care and genetics impact about 10 to 20% of your health outcome,” she said. Social services determine the rest.
“So basically our investments have been in the wrong place,” Novais said. “In Rhode Island, we’ve been trying to make that shift by moving our investments to be less disease-specific focused.”
Although some factors lie beyond its purview, the Health Department has begun moving in that direction with the establishment of Health Equity Zones in different regions of the state. First funded in 2015, the zones provide training and assistance to community health-care and social-service programs and leaders.
Also, the Health Department states, the zones allow “residents to join and lead broader efforts to eliminate barriers like poverty and repair injustices in systems such as education, health, criminal justice and transportation.”
Former state Health Director Dr. Michael Fine, now the Blackstone Valley Community Health Care senior clinical and population health officer, sees improved primary-care medicine as another key to improving health outcomes and lowering costs.
“We haven’t incentivized primary-care practices to maintain open access,” he said. “Too many people have the experience of calling their primary-care doctor because they have an earache and getting told, ‘Well, we have an opening in two weeks.’ That’s totally unacceptable.”
Primary-care practices should see patients the day they report a sickness, he said. And more primary-care physicians are needed, although the lower pay compared to such specialties as neurosurgery discourages many young doctors from entering the field.
“We need to create a culture in which everybody has and uses a primary-care doctor,” Fine said. “That’s the way it must be if we’re going to have an affordable health-care system.”
Rhode Island has not sufficiently addressed the environmental factors behind some poor health outcomes including asthma and cancer, Fine also contends. According to the Centers for Disease Control and Prevention, Rhode Island has the third-worst rate of adults with asthma (12.3% of the total adult population) and the 26th-worst rate of cancer mortality (154.2 deaths per 100,000 people).
Rhode Island’s long manufacturing history dating back to the late 1700s and Samuel Slater’s Pawtucket mill accounts for some of those damaging environmental factors, asserts Fine, author of “Health Care Revolt: How to Organize, Build a Better Healthcare System, and Resuscitate Democracy — All at the Same Time.”
“One hundred years ago, we were most industrialized state in the country,” Fine said. “Our air and water and buildings are still seething with toxic exposures.”
Dr. James E. Fanale, president and CEO of Care New England, the state’s second-largest healthcare system, sees a dichotomy.
“It’s nice that we have some of the best technology and science in the world here,” he said. “Very advanced. But when you look at the basic health of our community with vaccinations, infant mortality, et cetera, we don't hit it out of the park.”
According to Rhode Island Kids Count, the state’s infant mortality rate was 5.7 per 1,000 live births in 2016, 16th-best in the United States and a slight improvement from 2006 — but the rate for blacks worsened, to 11.5. The Commonwealth Fund reported that the rate of children ages 19 to 35 months who did not receive all recommended vaccines also worsened from 2012 to 2016.
Access is an issue, as is arranging services, said Fanale, who is a practicing geriatrician.
“I had a patient a few weeks ago who needed something,” he said. “I had to spend three hours on a Friday afternoon navigating with that person for what they absolutely needed — and I know how to get something. I feel badly for the poor person across the street that quote, unquote, has no clue.”
Unnecessary testing is another issue, Fanale said. He gave the example of doctors who conduct an EKG year after year on annual checkups.
“If you go back to your primary care doc next year and they do another EKG, I will tell you it's absolutely, totally, unambiguously useless,” Fanale said. “It has no value whatsoever. So we do a lot of low-value things that are unnecessary because unfortunately, ‘I'm running a business, too, as a physician. I get paid for it.’ ”
Similarly, Fanale said, some doctors comply with a patient’s request for a costly MRI when the patient is experiencing back pain. Not good practice, he said, in this age of people Googling for every ache and pain.
“We know that 90% of back pain goes away with time and [cost-effective] care,” Fanale said. “You need an MRI when nothing else works and you’re ready to go have it fixed surgically. So I tell my patients, ‘You want an MRI? Are you ready for surgery next week?’ ”
Dr. Timothy J. Babineau, president and CEO of Lifespan, Rhode Island’s largest health-care system, also stresses the importance of primary care as a means of reducing expensive emergency-department visits and hospitalizations. He agrees that good population health requires more than traditional medical care.
“Your zip code is more important than your genetic code in determining your health and well-being,” Babineau said. “We know the social determinants of health play a huge factor in a patient's overall health — among them, smoking, substance abuse, obesity, food deserts, housing security, gun violence.” And they play a corresponding role in life expectancy, which varies by community. According to the University of Rhode Island’s Rhode Island Life Expectancy Project, Barrington has the state’s highest life expectancy, 83.13 years; Woonsocket, at 75.85, has the lowest.
Still, as Babineau, Fanale, Fine, Novais and other experts agree, zip code is not necessarily destiny. Factors over which an individual has some control – among them, diet, exercise, sleep, weight, emotion and substance use – play roles in life expectancy.
Like Care New England and other systems, Lifespan is broadening its efforts to address these issues, Babineau said.
“We've had outreach in our community for years, but we're taking a more diligent and proactive approach to understand what role we need to play to create healthier communities,” Babineau said.
One element of Rhode Island’s health-care costs, Babineau said, is the large number of people age 65 and older who live here: 182,254 people, 17.24% of the population, placing Rhode Island 15th in the nation, according to the U.S. Census Bureau. Aging inevitably brings intensifying health needs.
A second is the relatively high price of labor in the Northeast. A third is the intrinsically greater expense of an academic system where research flourishes. Lifespan and Care New England have affiliations with the Warren Alpert Medical School of Brown University; Roger Williams Medical Center is affiliated with Boston University’s medical school. Other centers have other affiliations.
But this brings significant advantages, the Lifespan chief said.
“We may be a little bit more expensive, but when you come to an academic healthcare system, your chances of dying are less and your chances of having a complication are less.”
As the new head of the Executive Office of Health and Human Services, Womazetta Jones manages agencies including the Departments of Health; Children, Youth and Families; Behavioral Healthcare, Developmental Disabilities and Hospitals; and Human Services.
“What's very important is understanding the stressors that are on the shoulders of those who are really struggling for access and affordability,” Jones told The Journal. “The stress of that in and of itself does not lend itself well to better life outcomes or health outcomes.”
She gave the example of a family living in a food desert (an area where fresh, affordable, nutritious food is dificult to buy) and that has children in an inferior school, a description fitting many residents of Providence and other cities.
“If your nutrition isn't there or you’re stressing out because your children have to go to not-up-to-standard schools,” health is affected, Jones said. Stress can be toxic, science has demonstrated.
“If you keep adding more and more and more onto the shoulders of individuals who are struggling,” Jones said, “you can't expect even with the best health insurance to really change the tide of what the health outcome data is telling us.”
As she settles into her new job, Jones said a priority is better coordination among the departments she heads so that an individual can better “live healthy from the physical to the mental to the emotional — and to some, the spiritual.”
Her broad message?
“I rest on three pillars. Community engagement, racial equity, and how we treat the whole person. We need to maximize the dollars we have.”
Having been brought by ambulance to a hospital emergency department many times before being admitted, retired dental technician Witkowski is no fan of the process.
He said, half in jest: “You wait hours and you have to sign all kinds of stuff, they ask you about your insurance and this and that. You can be dead by the time you get in and they tell you what's wrong.”
And while he knows that a heart attack would require a readmission, the status quo today is much to his liking. Wife Thelma agreed.
“You feel more calm when you are home,” she said.
“No question at all,” said Witkowski. “That’s the biggest thing, mentally.”
“It sounds stupid,” his wife said, “but I feel like I’m sitting in a cloud and there are angels in back of us with their wings.”