
Midwives based outside rural areas they promise to serve
A GateHouse Media analysis of more than 3,000 midwives show most located in populated areas.
When non-nurse midwives lobbied Alabama lawmakers for licensure, they promised to help close the distance between pregnant women and their maternity providers — a gap that’s widening as rural hospitals and obstetric units close across the United States.
“They had ladies walking the statehouse with their babies in tow,” said Alabama state Sen. Larry Stutts, who opposed the legislation. “They said they were going to provide obstetric care in underserved areas of the state.”
The bill passed in 2017, and Alabama began licensing non-nurse midwives in January of this year.
But none of the newly licensed practitioners are located in so-called maternity care deserts. They’re all based in well-served areas.
The situation isn’t unique to Alabama.
Non-nurse midwives, who provide maternity care and deliver babies in homes and freestanding birth centers, have lobbied lawmakers for licensure and other rights across the country by promising to serve rural areas.
Proponents made the claim most recently in Kentucky, which in March passed its own bill to license and regulate non-nurse midwives.
But a GateHouse Media data analysis of more than 3,000 non-nurse midwives and freestanding birth centers shows the majority are clustered in cities and suburbs already served by hospitals with obstetric care units.
“That would be where people have more money and have better insurance,” said Linda Johnson, a retired certified nurse midwife from Michigan, which passed its own law in 2017 licensing non-nurse midwives.
Supporters of the Michigan bill used the same talking point, Johnson said. But lesser-populated counties accounted for just 15 percent of U.S. out-of-hospital births in the past decade, data from the Centers for Disease Control and Prevention show.
“Midwives are always saying they’re going to take care of these people nobody else wants, and that’s not what they do,” said Martha Reilly, an obstetrician-gynecologist near Eugene, Oregon. “They actually take care of the healthiest patients in the cities and the better-covered areas.”
An estimated 5 million women live in maternity care deserts, defined as a county with neither an obstetric provider nor a hospital offering obstetric care, according to the March of Dimes, which links lack of access to maternal mortality and poor birth outcomes.
Nearly 1,100 such deserts exist nationwide. Those numbers are likely to grow as rural hospitals continue to close their obstetric units or shut their doors entirely.
Some 200 rural counties lost hospital-based obstetric services between 2004 and 2014, the March of Dimes found.
And more than 100 rural hospitals have closed altogether since the beginning of the decade, according to the North Carolina Rural Health Research Program, which tracks the closures.
Still remaining are some 6,200 hospitals throughout the United States. Of them, 2,330 have obstetric care units, based on data from the American Hospital Association, which provided the locations to GateHouse Media for its analysis.
GateHouse collected the locations of freestanding birth centers and non-nurse midwives from state agencies and midwifery associations during its 2018 “Failure to Deliver” investigation on the rise and risks of out-of-hospital deliveries.
It identified 333 licensed and unlicensed freestanding birth centers across the country.
And it identified 3,055 midwives across the 36 states where data was available. Those states include both those that license and regulate non-nurse midwives and those that don’t.
When overlaying locations for all three — hospitals, birth centers and non-nurse midwives — the data show neither midwives nor freestanding birth centers fill the gaps some predicted they would.
Of the 2,224 counties in those states for which GateHouse Media had data for all three providers, 998 had hospital-based obstetric care, 1,021 had hospital-based obstetric care and a freestanding birth center and 1,145 had hospital-based obstetric care, a freestanding birth center and a non-nurse midwife. Birth centers and midwives filled a gap in just 12 percent of counties without hospital-based obstetric care.
Unlike the March of Dimes study, the GateHouse Media county-level analysis does not include obstetric providers outside of hospitals.
But out-of-hospital midwives don’t serve just the counties in which they live. Some travel great distances to reach far-flung clients.
Non-nurse midwife Venessa Giron told GateHouse Media last year she cared for women in as many as four contiguous states at one time.
“In northwest Arkansas, I literally am 15 minutes from Oklahoma, 30 minutes from Missouri and 45 minutes from Kansas,” said Giron, whose Arkansas license was revoked in 2016. She now is based in Oklahoma.
There’s no recommended safe driving distance between laboring mothers and their providers, whether that’s between a mother and her hospital or a midwife and her client.
Representatives for industry organizations contacted by GateHouse Media — the American College of Obstetricians and Gynecologists, the American College of Nurse-Midwives and the National Association of Certified Professional Midwives — could not point to any guidelines. The Midwives Alliance of North America did not respond to requests for comment.
Some states do regulate the distance between out-of-hospital births and the nearest hospital.
New York, for example, requires freestanding birth centers have a transfer agreement with a hospital no more than 20 minutes away. In Florida, a home-birth client’s distance from emergency care is considered a risk factor if it’s more than 30 minutes away.
But the regulations do not apply to the distance between midwives and their clients.
To view midwives and freestanding birth centers by area served — instead of just the county in which they are located — GateHouse Media converted minutes to miles and created a 30-mile and a 60-mile radius around each. That also revealed large areas without close access to midwifery care.
Using a 30-mile radius, major gaps still exist.
Using a 60-mile radius, gaps remain.
And distance matters.
As was the case in 2013 when Cape Girardeau, Missouri, midwife Joann Falcon agreed to deliver Andrea Smith’s twin girls in a home birth despite the roughly 115 miles between them.
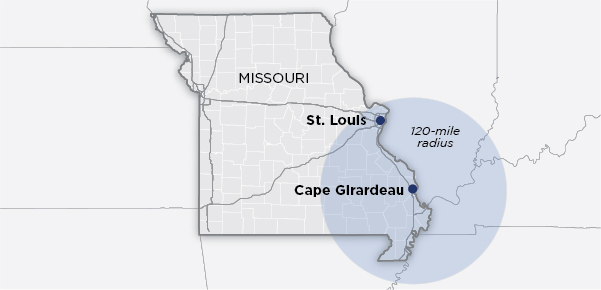
It took Falcon nearly two hours to get to Smith’s house the night she went into labor — enough time for one of the babies to suffer complications from a prolapsed umbilical cord, medical records show. The baby died three weeks later.
“At that moment in time, she should have just been, like, ‘I’m too far from you right now,’” Smith said in an interview last year.
In spite of cases like Smith’s, midwives continue to push for legislation and use provider shortages in rural areas as a talking point.
“Everybody is using this rural health care thing to increase their scope of practice. And it works, because all over the country, rural areas are having trouble getting health care,” said Ervin Yen, an anesthesiologist and former state senator in Oklahoma.
Yen tried two years in a row to regulate and restrict the practice of non-nurse midwives in Oklahoma but was unsuccessful each time. Currently, anyone can be a midwife in the Sooner State, regardless of education or training. No state agency oversees them.
Other lawmakers support the expansion of non-nurse midwives to serve needy areas despite the potential distance.
Michigan state Senator Ed McBroom, who sponsored the bill to license midwives, told colleagues in a 2015 legislative hearing that a midwife delivered all his children. He also said the midwife is located more than three hours away.
McBroom, who was then a state representative, said the state needs more midwives to serve rural areas.
The bill passed and was signed into law in 2017. The state has yet to begin licensing midwives, but GateHouse Media collected the locations of non-nurse midwives already practicing there from the Michigan Midwives Association in 2018.
The data show most of them are located in populous counties.

In Oregon, midwives are lobbying for a bill that would expand health insurance coverage for freestanding birth centers. The last action on the bill was a March 5 committee hearing.
Data show the majority of midwives in Oregon are clustered near Portland.

And in Alabama, where midwives said they would fill the gaps, the six practitioners who got their licenses this year all are located in highly populated counties — none of which are considered maternity care deserts.

No data exists yet for the location of non-nurse midwives in Kentucky, because they were banned there prior to the passage of this year’s law to license and regulate them.
But some say midwives aren’t the answer to the rural maternity care crisis in the first place.
“There are so many counties that don’t have a single health care provider. A big part of obstetric care is the prenatal care, preconception care and postpartum care,” said legislative chair for the Kentucky Section of the American College of Obstetricians and Gynecologists Jeffrey Goldberg. “Lay midwifery is not going to be a solution for that.”